Canine Myofascial Trigger Points: Unraveling The Mystery Of Fascia and Treatment of Myofascial Trigger Points
Ah, what a tangled web they weave, those fascia bundles!
Fascia is a network of connective tissue that surrounds body organs, muscles, groups of muscles, nerves, etc. It is a dense maze of collagen fibers that provide structure and support for these internal body parts.

My first semester of PT training involved literally tearing through the fascia layers to get to muscles and nerves. That experience was invaluable in understanding the feel and density of fascia. I developed a sense of what a patient would experience if that same tissue was tight or restricted. Ouch!
What is fascia?
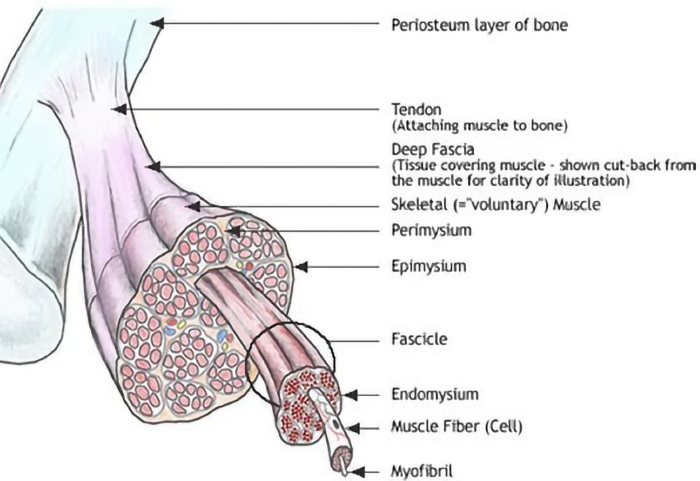
Fascia is physically prevalent surrounding muscles. The term “myo (meaning ‘muscle’) fascial” describes the type of pain syndrome that develops when it is traumatized.
Myofascial trigger points
Myofascial pain occurs from:
- any type of overload,
- repetitive motion
- fatigue
- direct injury such as compression or overstretching
- and due to exposure to cold/having a chill
The exact mechanism of pain is still speculative, but most medical folks believe it is mechanical in nature. In other words, it is not inflammatory or chemical and does not typically respond to anti-inflammatory medication.
It responds to treatment that is mechanical and physical in nature.
Myofascial pain is typically a chronic disorder. It is associated with tender and sensitive spots or zones in the muscle called trigger points.
These trigger points (MTrPs) can be either
- active or latent (in remission) and can cause pain either locally (at that direct spot)
- or in referred (in another location).\
Active myofascial trigger points
Active trigger points, or nodules, cause pain locally when compressed or pushed with your finger.
Latent myofascial trigger points
Latent myofascial trigger points cause pain in a different and seemingly unrelated, areas of the body when they are compressed.
Weird, right?
It becomes challenging when the patient cannot speak and subjectively identify the location of pain when you press on their trigger point!
Diagnosing myofascial trigger points
In veterinary medicine, myofascial pain syndromes with trigger points are a diagnosis of exclusion. It is important to rule out other things such as bone issues, joint, neurological status, etc.
Sometimes the diagnosis of myofascial pain with trigger points can only be surmised when tenderness and hardness of the tissue softens and disappears after animal treatment.
There are diagnostic tests available that measure pressure thresholds in soft tissues, as well as thermography which measures tissue heat. Use of x-rays and ultrasound are of no help indirectly diagnosing MTrPs.
Common pain patterns and body areas where myofascial pain with MTrPs can occur in animals:
- hips
- along the sides of the lumbar spine
- front thighs
- shoulder blades
- upper forelimbs
- etc.
Specific muscles in those areas that often have trigger points:
- the psoas
- quadriceps
- gracilis
- ileocostal lumborum
- infraspinatus
- triceps
- etc.
These muscles will feel shortened, tender and hypertrophied (enlarged or engorged) to touch, along with the presence of hard spots (MTrPs).
The dog may yelp or flinch when the MTrPs upon touch or pressure, or limp—to the point of total non-weight bearing in some cases.
Dogs might exhibit:
- head-bobbing during walking
- reluctance to walk or climb steps
- rounded posture with the head positioned downward or the rear end slumped and tucked in
The dog may stand with one shoulder higher than the other, or a hip hiked upward. That indicates the side involved with having active tripper points.
Treating myofascial trigger points
Treatment of this condition is best performed by clinicians having a high degree of knowledge in muscle anatomy with good palpation skills. That can include:
- physical therapists
- myofascial therapists
- massage therapists
- and chiropractors
Treatment of MTrPs involves:
- massage
- myofascial release
- electrical stimulation
- stretching (and a unique technique called “Spray and Stretch”)
- dry needling
- and trigger point injections
1. Massage
For trigger points, a special type of massage is used to reduce or deactivate the hardened nodule. Cross Friction is used with the hands moving in a perpendicular direction to the muscle fibers and other times the therapist uses their knuckles or elbow is used to defuse the barrier (called Prudden technique).
A myofascial release can also be performed with the hands in a light gliding motion to help unlock barriers in the fascia and with deeper pressure to mobilize muscle fibers and other soft tissues.
2. Electrical Stimulation
TENS (Transcutaneous Electrical Nerve Stimulation) and Interferential current are used with electrodes placed on the skin directly over the trigger points and including the areas of referred pain, to reduce the pain sensations. (Dogs with thick or long coats must be shaved)
The basis behind this treatment is “Gate Theory”. Electrical impulses from the stimulator block nerve pain signals at the spinal cord. This prevents them from reaching the brain and the sensation of pain decreases. It is similar to a human’s instinct to vigorously rub their elbow or foot is it is accidentally struck or stubbed. The rubbing provides a distraction and pain-blocking sensation.
3. Stretching
Stretching to the muscle where the MTrPs are located helps to elongate and physically break the pain cycle within the interlocking muscle fibers. The stretches are done initially by the therapist and can subsequently be taught to the pet owner.
4. Spray and Stretch
Fo muscles that don’t relax or yield to stretching, a special technique using an aerosol spray is used. This technique was originally developed in the 1950s by Dr. Janet Travell and is still used today with humans and animals!
TetraFluropethane or PentaFluropropane are non-flammable and non-ozone-depleting topical anesthetics. They are sprayed at an acute angle, 12-18 inch distance from the skin and speed of 4-5 inches per second, along the affected muscle while the therapist elongates it. The thin spray is a bit cold but most dogs are able to relax during the short treatment if they are spoken to gently and held firmly.
5. Dry Needling
Though sometimes confused for acupuncture, dry needling it is very different in procedure and purpose.
A thin filament needle (the same type that is used in acupuncture treatment) is inserted into the affected muscle and trigger point area, at a depth of 5-10mm, held for 30 seconds or so, sometimes “giggled” or vibrated slightly, for the purpose of mechanical disruption of knots. This needling procedure is usually repeated 5-6 times at each treatment session.
This is not a form of ancient Chinese medicine. It doesn’t treat disease, and does not use linear meridian pathways nor acupuncture points. Veterinarians can perform dry needling as well as physical therapists that practice in U.S. states or countries that allow them to use needles.
No medication is injected into the tissue and dry needling serves only to mechanically diffuse the trigger point.
6. Trigger Point Injections
Veterinarians can perform direct injection of trigger points with pain=reducing and/or anti-inflammatory medication. In human practice, medications used for this purpose include Dexamethasone, Lidocaine, Saline and Botulin Toxin.
In the veterinary field, the type of medication used for soft tissue injections varies, and your vet determines which is best.

