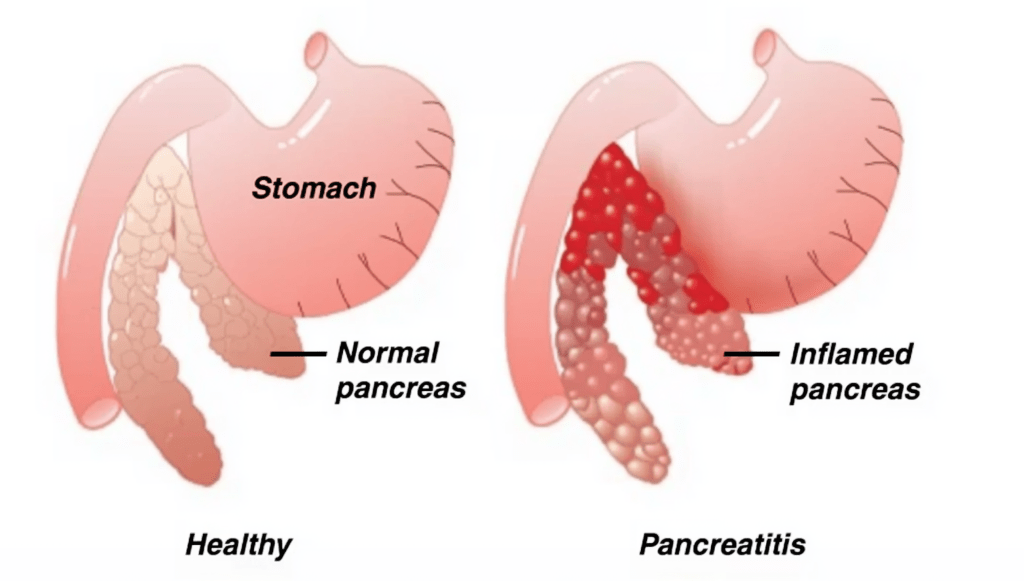
Canine Pancreatitis: What Causes It? Triggers Beyond Diet
The most common and well-known trigger for pancreatitis in dogs is a fatty meal or table scraps.
That’s why veterinary emergency clinics see a surge in cases during holidays, when rich foods abound.
But is the answer really that simple?
Why some dogs can raid the garbage, devour fatty bits, and stay perfectly healthy, while others fall severely ill after just a small piece of steak—or even nothing at all.
How can two dogs of the same breed, living in the same home and eating identical diets, have such different outcomes? One remains vibrant and symptom-free, while the other succumbs to severe acute or chronic pancreatitis? The truth is, pancreatitis in dogs is multi-factorial, influenced by genetics, underlying health conditions, and more.
Canine pancreatitis up close and personal
With my Rottweiler Cookie, I dealt with pancreatitis twice. Neither of the times it had anything to do with fat. The first time, Cookie got acute pancreatitis after helping herself to horse feed. Horse feeds contain grains, fiber, and additives. They are clearly not intended for dogs. The overload can spark pancreatic inflammation.
The second time, it was a complication of splenectomy. The surgery stresses the abdomen. Since the spleen sits near the pancreas, trauma or enzyme leaks can trigger the issues.
To note, Cookie’s blood work was always pristine, with no hyperlipidemia.

Canine Pancreatitis Symptoms
Symptoms can vary by severity and whether your dog suffers from chronic or acute pancreatitis. Dogs hide pain well, until becomes severe.
Chronic Pancreatitis
- reduced appetite
- occasional vomiting or diarrhea
- mild lethargy or tiredness
- subtle abdominal discomfort
- weight loss over time.
This signs are vague and mimic other issues
Acute Pancreatitis

Severe cases hit fast, with severe pain. Symptoms are not subtle and include:
- persistent vomiting
- severe diarrhea
- extreme lethargy or weakness
- sharp abdominal pain—dogs hunch or prayer position
- fever or dehydration
- collapse or shock
Infection spreads quickly. Organs fail without treatment.
With Cookie, the first sign was her looking dog tired. Way more tired that could possibly make sense. I was on full alert. Then she refused to eat. The first time she threw up, I was on a way to the vet. She didn’t eat anything fatty. Eventually we figured out the horse feed as most likely trigger.
Canine pancreatitis: Lack of Full Understanding
So what are the known risk factors, besides fatty meal(s) or table scraps?
Why can one dog’s pancreas deal with anything that gets thrown at it, while another breaks down? What makes one dog more vulnerable than the other?
In many dogs, pancreatitis develops when multiple risk factors overlap rather than from one single trigger. What are those risk factors? Let’s take a closer look:
Hyperlipidemia
Hyperlipidemia — an excessive amount of fat molecules (lipids) in the blood — is strongly associated with episodes of pancreatitis.
Interestingly, it isn’t always clear what comes first: the chicken or the egg. Or in this case, hyperlipidemia or pancreatitis. Elevated blood lipids can increase the risk of pancreatitis, but pancreatitis itself can also disrupt fat metabolism, leading to elevated lipid levels.
In many dogs, hyperlipidemia develops secondary to other underlying disorders, such as:
- diabetes mellitus
- hypothyroidism
- Cushing’s disease
- some liver diseases
- kidney disease
Some dogs, however, develop primary hyperlipidemia, where no underlying disorder can be identified.
And yes — high-fat foods can contribute to hyperlipidemia, particularly in dogs already predisposed to abnormal fat metabolism.
Breed predisposition
Though any dog can develop pancreatitis, genetics often play a role. Certain breeds are at higher risk, in part due to inherited tendencies toward hyperlipidemia — elevated fat levels in the blood.
Breeds commonly associated with increased risk include Miniature Schnauzers, Miniature Poodles, and Cocker Spaniels. For example, Miniature Schnauzers have up to 20-30% higher risk of getting pancreatitis compared to other breeds.
Other breeds that appear more frequently in studies include Yorkshire Terriers, Cavalier King Charles Spaniels, Dachshunds, Boxers, Collies, and Skye Terriers.
Terrier breeds as a group also carry increased risk. This includes Australian Terriers and Bedlington Terriers.
Obesity
Yes, folks, here it is again. Overweight dogs are more susceptible to pancreatitis. Excess stored fat raises blood lipid levels, which, as noted above, are closely linked to pancreatic inflammation.
Spayed and neutered dogs may be at especially high risk. Hormonal changes can slow metabolism in females and increase appetite in males, making weight management more challenging.
Over time, this combination of increased fat storage and altered metabolism can contribute to conditions that place additional strain on the pancreas.
Stress
High stress can be a contributing factor too. Stress isn’t just an emotional experience — it triggers real, measurable changes in the body.
When a dog is in a prolonged fight-or-flight state, stress hormones such as cortisol and adrenaline are released. These hormones affect metabolism, digestion, blood flow, and inflammatory responses. Over time, this can disrupt normal digestive regulation and place additional strain on organs involved in metabolism, including the pancreas.
Stress alone is unlikely to cause pancreatitis. However, ongoing or intense stress may reduce the body’s ability to maintain balance, making the pancreas more vulnerable — particularly when other risk factors are already present.
Stressors can include major life changes such as re-homing, boarding, surgery, or hospitalization, as well as chronic anxiety, pain, illness, or repeated stress that never fully resolves.
Metabolic disorders
There is a higher incidence of pancreatitis in dogs with metabolic disorders such as diabetes mellitus, Cushing’s syndrome, and hypothyroidism.
These conditions affect how the body regulates blood sugar, hormones, and fat metabolism. As a result, they are commonly associated with hyperlipidemia — elevated fat levels in the blood — which is a known risk factor for pancreatitis.
In dogs with metabolic disease, the pancreas may already be under increased metabolic demand. When normal regulatory balance is disrupted, the pancreas can become more vulnerable to inflammation, particularly if additional triggers such as dietary fat, obesity, stress, or illness are present.
Managing the underlying metabolic condition is an important part of reducing overall risk and supporting pancreatic health.
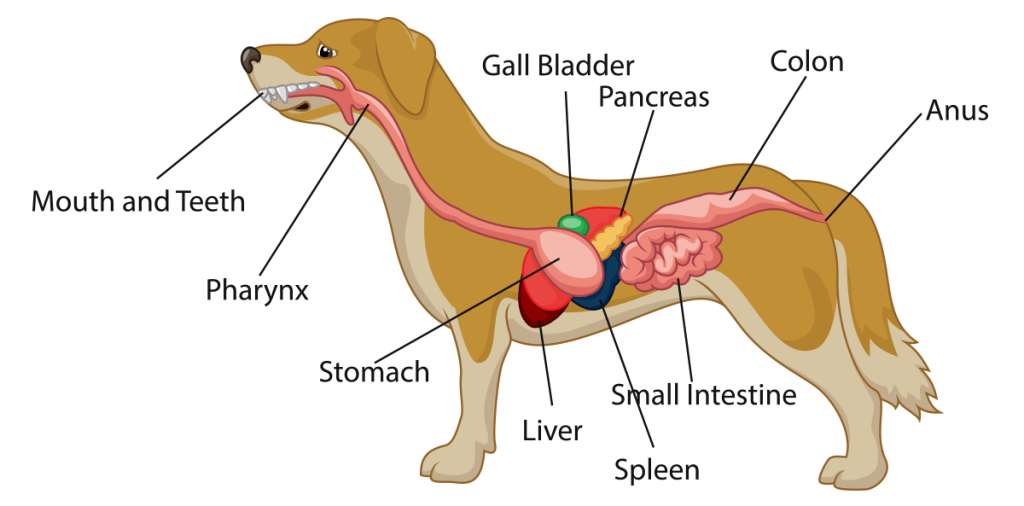
Reflux of duodenal contents
The duodenum is the first section of the small intestine. It is where bile from the liver and digestive enzymes from the pancreas are released to help break down food.
Under normal circumstances, pancreatic enzymes are produced in an inactive form and are only activated once they enter the duodenum. This timing is critical — it prevents the pancreas from digesting itself.
If duodenal contents reflux, or back-wash, into the pancreas, those enzymes can become activated too early. When this happens, digestive enzymes may begin damaging pancreatic tissue instead of food, triggering inflammation.
This premature enzyme activation is believed to play a role in the development of pancreatitis and helps explain why conditions that disrupt normal digestive flow can increase risk.
Drugs and toxins
Certain drugs or toxins increase the risk of pancreatitis
Medications that can predispose dogs to pancreatitis include certain antibiotics, anti-seizure medications, and some chemotherapy agents. These drugs can affect metabolism, inflammation, or pancreatic function, increasing vulnerability in susceptible dogs.
The role of corticosteroids remains controversial. However, if naturally elevated cortisol levels — as seen in Cushing’s disease — increase pancreatitis risk, it is reasonable to consider that corticosteroid medications may contribute as well, particularly with higher doses or long-term use.
Exposure to certain toxins has also been linked to pancreatitis. Organophosphate insecticides, in particular, have been implicated.
Trauma to the pancreas or a tumor
Anything that physically disrupts normal pancreatic tissue can trigger the inflammation at the heart of pancreatitis.
Direct trauma to the abdomen, surgical manipulation, or injury to nearby organs can irritate the pancreas. Because the pancreas sits close to the stomach, intestines, liver, and spleen, inflammation or trauma in one area can easily affect another.
Abdominal surgery, blunt trauma, or complications that alter blood flow or allow digestive enzymes to leak can all place stress on pancreatic tissue. Tumors in or near the pancreas can have a similar effect by compressing tissue, disrupting normal drainage, or interfering with local circulation.
In these situations, pancreatitis develops not because of diet or metabolism, but because the pancreas has been physically disturbed or compromised.
Hypercalcemia
Excessive levels of calcium in the blood can interfere with normal pancreatic function by prematurely activating digestive enzymes that are meant to remain inactive until they reach the intestine.
Under normal conditions, pancreatic enzymes stay safely stored in an inactive form inside the pancreas. Calcium plays a role in enzyme activation, and when blood calcium levels rise abnormally, that control can break down. Elevated calcium can trigger enzyme activation inside pancreatic cells instead of in the duodenum, allowing digestive enzymes to begin damaging pancreatic tissue.
This process sets the stage for inflammation and helps explain how pancreatitis can develop even in the absence of dietary fat or other common triggers.
Hypercalcemia itself is usually a secondary problem rather than a primary one. Common causes include:
- vitamin D poisoning
- certain cancers
- parathyroid dysfunction
- kidney failure
- Addison’s disease
In these cases, pancreatitis may emerge as a downstream complication of a broader metabolic disturbance.
Autoimmune in origin
In some cases, chronic inflammation may trigger an abnormal immune response that targets pancreatic tissue itself.
Emerging research suggests that immune-mediated mechanisms can play a role in certain forms of chronic pancreatitis. Instead of resolving inflammation, the immune system continues to activate, leading to ongoing tissue damage and progressive loss of pancreatic function.
This process does not appear to be common, and it is not always easy to identify. However, it may help explain why some dogs develop chronic or recurrent pancreatitis without obvious dietary, metabolic, or mechanical triggers.
Unrelated health issues
The pancreas is not an island.
In chronic or recurrent cases of pancreatitis, problems elsewhere in the body can influence pancreatic health. The function of other organs — particularly those involved in digestion and metabolism — often needs careful evaluation.
Conditions such as inflammatory bowel disease (IBD), as well as liver, gallbladder, and kidney disease, can all play a role. Inflammation, impaired bile flow, altered digestion, or metabolic strain in one organ system can place additional stress on the pancreas.
In these cases, pancreatitis may not exist in isolation, but as part of a broader pattern of systemic or gastrointestinal disease.
Antioxidant deficiencies
Some human studies suggest that antioxidant deficiencies may play a role in chronic pancreatitis.
The pancreas is particularly sensitive to oxidative stress — damage caused by an imbalance between free radicals and the body’s ability to neutralize them. Antioxidants help limit this damage. When antioxidant defenses are insufficient, inflammatory processes may become more difficult to control, allowing ongoing tissue injury.
In chronic pancreatitis, repeated or unresolved inflammation can gradually overwhelm protective mechanisms. In this context, inadequate antioxidant support may contribute to disease persistence rather than act as a primary trigger.
Evidence in dogs remains limited, and antioxidant deficiency is unlikely to cause pancreatitis on its own. However, it may influence disease progression in dogs already dealing with chronic inflammation or other risk factors.
Scorpion stings
This is a rare trigger, but one worth mentioning for dogs living in regions where scorpions are common.
Scorpion venom can trigger intense systemic inflammation and has been associated with pancreatic inflammation in both humans and dogs. The venom affects the nervous system and can disrupt normal enzyme regulation, potentially leading to premature activation of pancreatic enzymes.
While scorpion stings are an uncommon cause of pancreatitis, they serve as a reminder that toxic and inflammatory insults — even brief ones — can affect the pancreas under the right circumstances.
Unknown causes
And then there are dogs who develop pancreatitis and no one ever figures out why.
Some dogs likely live with undiagnosed, low-grade chronic pancreatitis, flaring quietly or intermittently until something finally brings it to the surface. Others experience a single acute episode with no clear trigger, even after thorough testing.
Despite everything we know about risk factors and mechanisms, pancreatitis doesn’t always offer clean answers.
And then, of course, there is Cookie who got pancreatitis after getting into horse feed.
Pancreatitis is not a Simple Problem
Pancreatitis in dogs rarely has a single cause. Genetics, metabolism, health status, stress, medications, and chance all play a role.
That said, one risk factor is easy to control. Before offering your dog fatty scraps or rich foods, think twice. Avoiding high-fat treats and table scraps remains one of the simplest and most effective ways to reduce pancreatitis risk — especially in dogs that may already be vulnerable.
How Will Your Veterinarian Diagnose Pancreatitis?
Diagnosing pancreatitis can be challenging. No single test provides a definitive answer in every case.
Veterinarians typically rely on a combination of factors, including:
- clinical signs and history
- blood work, including pancreatic-specific tests
- imaging, such as abdominal ultrasound
Some dogs show clear laboratory abnormalities, while others have relatively normal results despite active inflammation. This is one reason pancreatitis can be difficult to diagnose, especially in mild or chronic cases.
SNAP cPL Test
Veterinarians now commonly use a canine pancreatic lipase (cPL) test to help diagnose pancreatitis in dogs.
cPL measures a pancreatic-specific enzyme released into the bloodstream during pancreatic inflammation. Because it targets lipase produced by the pancreas itself, it is more specific than older amylase or lipase tests.
An elevated cPL level increases suspicion for pancreatitis and is especially useful in moderate to severe acute cases. SNAP cPL tests offer rapid, in-clinic screening for symptomatic dogs, while laboratory cPL tests provide more precise measurements.
However, the cPL test is not perfect.
- Mild or chronic pancreatitis may not always cause a marked cPL elevation
- Some dogs with elevated cPL have no clinical signs
- cPL does not reliably distinguish between acute and chronic pancreatitis
- Results must be interpreted in context
For these reasons, cPL is best viewed as one piece of the diagnostic puzzle, not a standalone answer.
Treatment of Canine Pancreatitis
Treatment depends on severity and whether the condition is acute or chronic.
In acute cases, treatment often focuses on:
- pain control
- intravenous fluids
- anti-nausea and anti-vomiting medications
- supportive care
Severe cases may require hospitalization and close monitoring.
Chronic pancreatitis is typically managed rather than cured. Long-term care may include:
- dietary modification
- managing underlying conditions
- avoiding known triggers
- ongoing monitoring
The goal is to reduce inflammation, prevent flare-ups, and support overall quality of life.
Emerging Research and Evolving Care
Research into canine pancreatitis continues to evolve, particularly in the areas of targeted treatment and improved diagnostics. While supportive care remains the foundation of treatment, several newer approaches are under investigation.
Recent developments include:
- Targeted anti-inflammatory therapy
One of the most noteworthy recent developments is the conditional FDA approval of fuzapladib sodium (Panoquell-CA1) for treating acute pancreatitis in dogs. This drug acts as an LFA-1 inhibitor, reducing neutrophil activation and limiting inflammatory damage in the pancreas, and has shown clinical benefit in acute cases.
Source: Management of pancreatitis in dogs and the role of PANOQUELL®-CA1 (fuzapladib sodium for injection) - Experimental treatments under study
Researchers are studying novel approaches aimed at reducing the severity and mortality of pancreatitis in dogs. One investigational class includes pancreatic lipase inhibitors, designed to limit harmful enzyme activity during acute episodes. Early research has explored compounds such as RABI-767 in clinical settings, though these remain experimental and are not yet part of standard care.
For example, early findings and trial information can be found through clinical trial registries and veterinary research summaries. - Advances in diagnostics and biomarkers
Research is ongoing into new biomarkers that may help assess pancreatitis severity and prognosis in dogs. In addition to pancreatic lipase testing, studies are investigating markers such as pancreatic alpha-amylase (P-AMY), C-reactive protein (CRP), and inflammatory cytokines to provide more nuanced insight into disease activity and systemic response. These biomarkers could improve clinicians’ ability to track inflammation and guide treatment decisions over time.
Advances in the diagnosis of acute pancreatitis in dogs - Genetic and risk-factor research
Studies are examining genetic variants in certain breeds and how inherited risk may interact with environmental or metabolic triggers rather than act alone — for example, research into SPINK1 gene variants in Miniature Schnauzers found that the variant is common in the breed but not clearly linked with clinical pancreatitis.
High Prevalence of the c.74A>C SPINK1 Variant in Miniature and Standard Schnauzers
These developments are promising, but most are still emerging. They highlight progress in understanding pancreatitis — while reinforcing that it remains a complex disease without a single cause or cure.
Canine Pancreatitis FAQ
Yes. While fatty meals are a common trigger, many dogs develop pancreatitis due to metabolic disorders, medications, stress, surgery, trauma, or other underlying health conditions. Some cases remain unexplained.
Dogs vary widely in genetic risk, fat metabolism, hormone balance, and pancreatic sensitivity. What one dog tolerates easily may overwhelm another dog’s pancreas.
Stress alone is unlikely to cause pancreatitis, but prolonged or intense stress can disrupt metabolism and inflammatory regulation, making the pancreas more vulnerable—especially when other risk factors are present.
No. Some dogs experience a single acute episode, while others develop chronic or recurrent pancreatitis. Chronic cases may involve ongoing low-grade inflammation that flares periodically.
Yes. Abdominal surgery, trauma, or injury to nearby organs can physically stress the pancreas or disrupt normal enzyme regulation, triggering inflammation.
Yes. Some dogs develop pancreatitis without obvious abnormalities such as hyperlipidemia. Normal bloodwork does not rule out pancreatic inflammation.
No. While avoiding high-fat foods reduces risk, pancreatitis is a multifactorial condition. Some cases occur despite careful management and have no identifiable cause.
Seek veterinary care if your dog shows persistent vomiting, severe lethargy, abdominal pain, loss of appetite, or sudden collapse. Acute pancreatitis can escalate quickly.
Related articles:
Pancreatitis in Dogs: The Perplexities of Pancreatitis
Acute Pancreatitis in a Dog: The Project That Is Cookie—Pancreatitis Up Close And Personal
Severe Acute Pancreatitis in a Dog: Bandit’s Last Treat
Further reading:
Pancreatitis in Dogs
Pancreatitis in Dogs: Signs, Causes and Treatment
Decoding Pancreatitis with Dr. Kuzi